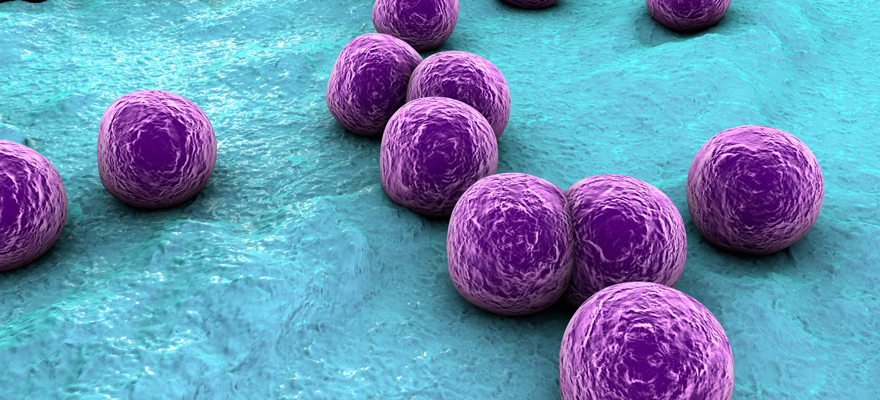
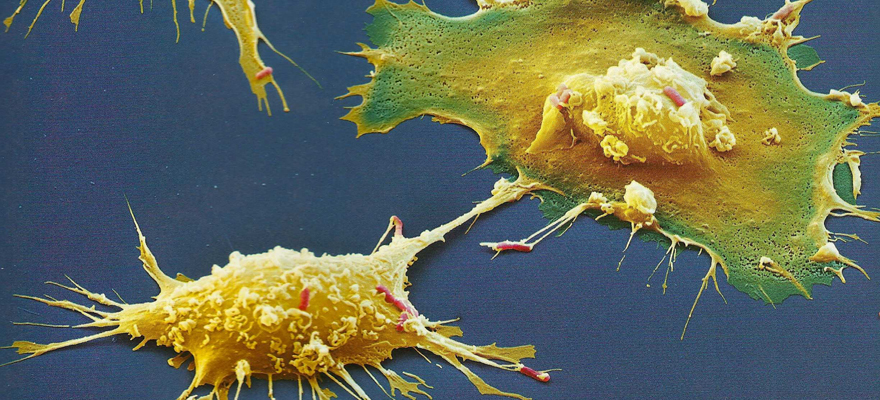
Microbes and Infections
We live surrounded by microorganisms like bacteria, viruses, fungi, and parasites, many of which can cause infectious diseases. Despite the availability of hundreds of antibiotics, antivirals, antifungals and vaccines, infections are still one of the most common causes of death worldwide. The problem is even escalating as the number of susceptible hosts increase and virulent, more resistant microbial strains emerge. According to estimates, the number of deaths from infections will exceed those from cancer in a few decades.
Infections are a significant cause of morbidity and mortality in patients with defective immune response such as those with cancer-related immunosuppression, organ transplantations, induced immunodificiencies, and neonates. Hospitalization in the intensive care unit may increase the risk for such infections.
Antimicrobial Resistance
Drug resistance is a natural phenomenon that, however, dramatically escalated since the 1990s - the golden era of antibiotics. When microorganisms are exposed to antimicrobial drugs, the more susceptible are annihilated while the more resistant ones may survive and transfer their resistance genes to their offsprings. Previously curable infectious diseases may become untreatable and spread throughout the world.
Worldwide inappropriate use and misuse of antimicrobials and poor quality medicines in developing countries exacerbated the problem as well as the use of sub-therapeutic doses of antibiotics in animal-rearing as growth promoter and for preventing diseases. Resistant microorganisms can spread via the environment and from animals to humans.
The occurence and spread of (multiple) antibiotic resistant bacteria is now an issue of global concern. An overview on the threat of antimicrobial resistance can be found
here.
With increasing pathogen resistance to antibiotics, population ageing, the threat of pandemics and the absence of fresh 'magic bullets' from the pharmaceutical industry there is a strong interest in the development of new approaches for the prevention and treatment of infectious diseases. In an effort to decrease our dependence on antimicrobials, non-antibiotic, albeit immune response enhancing substances will be of primary interest.
Our body protects itself from infectious agents and the damage they cause by a variety of specialized cells and molecules which together make up the immune system. Its main task is the recognition and elimination of pathogens without attacking the host's own healthy tissues. In most cases the immune system is working perfectly and eliminates pathogens without the outbreak of an infectious disease. However, in certain conditions physicians want to stimulate the anti-infective characteristics of the immune system.
The immune system of higher vertebrates is multilayered and consists of two main components: the innate and the adaptive immunity.
Innate Immunity
The innate immune system is a universal and ancient form of host defense. It is the first line of defense against a variety of pathogens and not specific for any individual pathogen.
If microorganisms penetrate into the body, antimicrobial peptides are released and disrupt the membranes of many microbes. Toll-like receptors and Nod-like receptors on blood cells recognize microbial structures and generate signals for the activation of host response. Macrophages engulf and digest pathogens, cytokines and chemokines are released and recruit phagocytes to infected tissues which ingest and kill invading microbes. Natural killer cells recognize and bind infected host cells and induce their apoptosis.
Most potential infections are warded off by the innate immune system within minutes to a few hours without causing disease symptoms. However, when microbes successfully avoided killing by the first defense lines, dendritic cells of the pathogen-specific innate immune system mobilize and instruct the more slowly developing mechanisms of antigen-specific adaptive immunity.
Adaptive Immunity
The adaptive (acquired) immunity can overcome pathogens that have evaded innate immunity. Compared to the innate immunity, the adaptive immune system is capable of eliminating infections more efficiently due to very specific recognition functions of white blood cells. These lymphocytes can recognize and respond to virtually any foreign structure by means of highly specialized antigen receptors on their surface.
Antibodies and activated lymphocytes produced by an adaptive immune response are very precise and efficient tools to eliminate pathogens and other foreign structures. They can persist after the original infection has been eliminated, allowing a faster and more intense response to a second exposure even years later. The characteristics of the adaptive immune system are applied in vaccinations since 1796 when Edward Jenner demonstrated that inoculation with cowpox could protect against smallpox.